Whilst looking for correlations on some other things, I fell across this important information that didn't make an impression on me then but it certainly does now. I guess it shows that it's a good practice to go back with the new ideas that you've gained and look at the data again.
Even though, by my estimates, there are millions of Ketosis Prone Diabetics out there, we remain the "mystery meat" of diabetics. There is very little research about its genesis. There is no way to identify a KPD before a diabetic emergency occurs. In fact, as far as I know, very few people are diagnosed as KPD even after they have had an extreme glycemic event and recovered. We don't even know what the numbers are for KPD. I tend to believe that an A1c greater than 10 with spikes above 300 is a good indicator, especially if the fasting blood sugar was less than 140 in the previous year. That thinking and two bucks might get you a cup of coffee.
We aren't high on anybody's list of things to do. So, I think it's important to glean what facts I can from whatever data is out there to help people deal with KPD. This brings up this little fact. It has to do with the tipping point or when does KPD go from being just a type of diabetes to something that can be deadly.
Ketosis-Prone Type 2 Diabetes in Patients of Sub-Saharan African Origin
Clinical Pathophysiology and Natural History of -Cell Dysfunction and Insulin Resistance
Franck Mauvais-Jarvis,1 Eugene Sobngwi,1 Raphae¨ l Porcher,2 Jean-Pierre Riveline,3
Jean-Philippe Kevorkian,4 Christian Vaisse,5 Guillaume Charpentier,3 Pierre-Jean Guillausseau,4
Patrick Vexiau,1 and Jean-Francois Gautier1
This is a study that tracks KPD's over ten years and compares them to regular Type 2's and Ketosis Prone Type 1's. This study is out of Paris done on emigrants who come mostly from Sub-Saharan Africa. I have talked or corresponded with people who question the relevance of this research to them because they aren't remotely African or descended from Africans. As I said before, this syndrome has been documented almost every. The research is very spare and I've had to cobble data from all over the world. I suggest that beggars can't be choosy. My position is that
anything that says
anything about KPD is relevant to all KPD's irrespective of color or origin.
ADA Criteria for the diagnosis of diabetes
1. A1C 6.5%. The test should be performed in a laboratory using a method that is NGSP certified and standardized to the DCCT assay.*
OR
2. FPG 126 mg/dl (7.0 mmol/l). Fasting is defined as no caloric intake for at least 8 h.*
OR
3. Two-hour plasma glucose 200 mg/dl (11.1 mmol/l) during an OGTT.
Standards of Medical Care in Diabetes—2010
http://care.diabetesjournals.org/content/33/Supplement_1/S11.full.pdf+html
That being said, let's get on with it. Above I have copied the ADA guidelines for diabetes diagnosis. It's important to keep these numbers in mind. It is especially important because, as I've said, most docs have no idea about how this works so you need to look out after your needs or those you know.
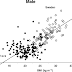
Buried in the KPD paper is a graph that describes the path that relapse takes in KPD's. Though it describes relapse, I am looking at it as just the course which KPD's take before their blood sugars go awry. What is my evidence for this. Well, there is one thing but I'll get to that later. Of course, A KPD, by definition, has already been diagnosed so it very definitely pertains to those.
What they found was that the course before relapse could be predicted by A1c over a years time. I tried to get this but it wouldn't copy. You can find it on page 650. Here's what they had to say.
The median duration between the development of hyperglycemia (HbA1c 6.3%) and the onset of a ketotic relapse was 12 months (95% CI, 6–21, Kaplan-Meier). During this period, the insulin secretory reserve, measured before the onset of hyperglycemia and during readmission for relapse, dramatically deteriorated ( C-peptide, 2.88 0.21 vs. 0.19 0.08 ng/ml; P 0.05). There was no precipitating illness other than hyperglycemia. The increase in HbA1c 6.3% was associated with an increased risk of ketotic relapse with an HR of 38 (95% CI, 5–286; P 0.0004). Thus, hyperglycemia preceded and was strongly associated with
the subsequent development of an insulin-deficient, ketotic relapse.
The chart is pretty clear. It tracks the A1c for 40 months. The A1c stays steady at around 6.3% and at about 12 months before relapse takes a slight jog up. At 6 months, it takes another jog up to about 6.6 %. From this point on, the curve becomes steep.
What you can see is that below 6.3% blood sugars remained steady. Above that number events go bad very quickly. The 6.3% averages out to a blood sugar of 134. The first jog up appears to be about 6.5%, which averages to daily blood sugar of 140. This 140 is not a random number. It is thought to be the point at which blood sugars become damaging and bring on long term complications.
My thought on this as occurring before the first episode is from some reading, which I can't find, that said it was frequent, that previous to diagnosis, a KPD would have a normal or near normal blood sugars 6 months before. This graph shows something similar. We have no idea what causes this catastrophe but the fact that its beginnings sit at this critical juncture seems to suggest that something gets broken here. What you have to recognize is that this is for people who've already broke down then gone into remission, so whatever got broken got fixed once the blood sugars were brought down.
Now look at the ADA guidelines. They've tightened them up but look how close they are to the KPD danger point. This guideline is really for T2's. Would you give this as a guideline for KPD's knowing that they can crash very quickly? If you are a KPD should you feel safe with these guidelines?
If you showed up at a doc with these numbers, the ADA recommends that the physician should inform you that you're prediabetic and that maybe you should start making adjustments with diet and exercise. You would be asked to return in 6 months for a checkup to see how things were going. This wouldn't be a problem for a Type 2 because onset isn't abrupt and acute but for a KPD these numbers should be sending off all types of alarms because in 6 months you could very well be hospitalized or at worse, dead.
Until there is a diagnostic test for KPD, we will continue to windup in emergency. For those who already know what they are; keep and eye on your blood sugars because, unlike a T2, whose numbers trend steadily, you can go off the rails very quickly.